India & World UpdatesHappeningsBreaking NewsFeature Story
Medical Inflation in India: A Growing Concern, written by Dr. Manoj Kumar Paul

//Dr. Manoj Kumar Paul//
Medical inflation refers to the sustained increase in the cost of healthcare services, including hospital care, diagnostic tests, treatments, pharmaceuticals, and insurance premiums. Unlike general inflation, which affects a wide array of goods and services, medical inflation specifically tracks the rising cost of accessing healthcare facilities and treatments. Over the past decade, this trend has accelerated, placing substantial financial and social pressure on households, insurers, and policymakers.
In 2024, medical inflation reached 14%, one of the highest in Asia, surpassing countries such as China, Japan, and South Korea. Projections for 2025 indicate a rate around 13% (Onsurity, 2025; Financial Express, 2025). Approximately 63% of Indian households continue to rely on out-of-pocket expenditures (NSSO), which exposes families to significant economic vulnerability.
Key factors contributing to this rise include the increasing prevalence of non-communicable diseases (NCDs), expansion of advanced medical technology, high costs of imported equipment, and limited regulation of drug prices. Additionally, demographic shifts, such as urban migration, aging populations, and changing lifestyles, have introduced more complex healthcare demands.
Understanding medical inflation is essential not only for economic planning but also for ensuring equitable access to healthcare, protecting household finances, and designing sustainable insurance and public health policies.
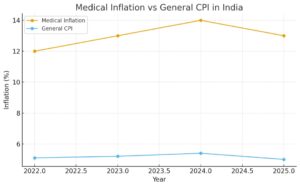
Monthly data provides further insight. In August 2025, healthcare inflation stood at 4.4%, nearly double the general CPI of 2.07%. Urban centers face even higher rates due to concentration of specialized hospitals, expensive diagnostics, and advanced treatments. Rural regions, while cheaper, often lack access, indirectly increasing travel and treatment costs.
Current Trends in Medical inflation:
Medical information has consistently outpaced general consumer price inflation in India, creating growing concerns for households, insurers, and government programs. In 2024, healthcare costs rose 14% against a general CPI of 5.5%, highlighting the disproportionate burden on households (MOSPI, 2025). The projected figure for 2025 is 13%, still above the global average of 10% (Financial Express, 2025).
Drivers include an increase in chronic illnesses, higher adoption of high-cost diagnostic equipment, and shortage of trained medical personnel. The rise of medical tourism has also fueled domestic price escalation, as hospitals upgrade services to meet international standards. Moreover, regulatory inconsistencies in drug pricing and equipment import duties exacerbate cost pressures.
These trends underscore the urgency for cost containment strategies, insurance coverage expansion, and systemic reforms to prevent further economic and health inequalities.
Financial Impact on Households
The financial consequences of medical inflation on Indian households are profound. Approximately 62% of hospital costs are paid directly by patients, while 23% are financed through loans, credit, or informal lending (Onsurity, 2025). High out-of-pocket expenditures often force families to postpone treatment, compromise on quality, or incur long-term debt.
Annually, 6–7% of households descend below the poverty line due to medical expenses, emphasizing the socioeconomic impact. Average hospitalization claims increased from ₹62,548 in FY 2022–23 to ₹70,558 in FY 2023–24, reflecting higher physician fees, extended stays, advanced diagnostics, and surgical costs (Business Standard, 2024).
Debt from medical spending reduces savings, curtails expenditure on education and nutrition, and heightens vulnerability to economic shocks. Even households with insurance are not immune; coverage gaps, exclusions, and high deductibles limit protection. Long-term solutions require enhanced insurance penetration, regulation of costs, and accessible healthcare for low-income families to mitigate financial distress.

Key Drivers of Medical Inflation
Several interrelated factors underpin medical inflation in India:
1. Technological Advancements: Innovations such as AI-based diagnostics, robotic surgeries, and advanced imaging improve outcomes but increase costs. Hospitals pass on expenses for equipment, maintenance, and staff training to patients (Onsurity, 2025).
2. Chronic Disease Prevalence: Conditions like diabetes, hypertension, and cardiovascular disorders demand continuous monitoring and medication. As per the Indian Council of Medical Research (ICMR, 2025), diabetes prevalence among adults has reached 8.3%, adding to recurrent expenses.
3. Hospital Operational Costs: Rising salaries for medical staff, infrastructure maintenance, and procurement of imported equipment drive up treatment prices.
4. Policy and Regulatory Factors: Inconsistent drug price controls, variable insurance reimbursements, and import duties on medical devices contribute to cost escalation. Delays in implementing reforms often allow inflation to persist.
5. Demographics and Urbanization: The aging population and urban lifestyle shifts elevate demand for high-quality healthcare, keeping treatment costs high.
Together, these factors create sustained upward pressure on healthcare costs, challenging affordability across socioeconomic groups.
Health Insurance and Medical Inflation:
Rising medical inflation directly impacts the health insurance sector. Premiums are increasing 15–20% annually, outpacing general inflation (Acko, 2025). Major drivers include higher hospitalization costs, prevalence of chronic diseases, adoption of expensive treatment technologies, and skilled personnel fees.
Regulatory initiatives, such as the National Health Claims Exchange (NHCE), standardize treatment rates, reduce billing discrepancies, and enhance claim transparency, helping insurers control costs (Reuters, 2025).
Insurance companies are adapting with preventive care programs, wellness incentives, co-payment structures, and data-driven risk assessment models. Despite these measures, persistent medical inflation challenges the balance between comprehensive coverage and affordability, underscoring the need for policy coordination and effective cost control.
Policy Measures and Government Initiatives:
The government has adopted multiple measures to curb medical inflation and improve affordability:
Pradhan Mantri Jan Arogya Yojana (PM-JAY): Provides up to ₹5 lakh per household per year for secondary and tertiary care, reducing OOP expenditure (National Health Authority, 2025).
National Health Claims Exchange (NHCE): Standardizes hospital pricing, regulates insurance claims, and prevents inflated billing (Reuters, 2025).
Medical Education Expansion: In 2025, 10,023 new MBBS and postgraduate seats were added to increase the supply of healthcare professionals, improving doctor-to-patient ratios, reducing consultation fees, and enhancing access in urban and rural areas (Ministry of Health and Family Welfare, 2025).
These initiatives demonstrate a multi-pronged approach, combining financial protection, workforce expansion, and regulatory oversight to contain medical inflation and enhance healthcare access.
Coping Strategies for Individuals:
Households can adopt layered strategies to mitigate the impact of rising medical costs:
1. Comprehensive Health Insurance: Policies covering hospitalization, outpatient care, pre-existing conditions, and critical illnesses reduce financial burden. Add-ons such as maternity, dental, and wellness programs improve protection. Evaluating network hospitals, claim settlement ratios, and exclusions ensures cost-effectiveness.
2. Preventive Healthcare: Routine check-ups, chronic disease screenings, timely vaccinations, and lifestyle measures like balanced diet, physical activity, and stress management help detect health issues early, avoiding expensive interventions.
3. Government Schemes: Utilizing PM-JAY and similar programs for eligible households lowers financial exposure. Awareness of scheme eligibility and benefits maximizes protection.
4. Financial Planning: Maintaining an emergency health fund, budgeting for routine medications, and setting aside premiums ensure preparedness for unexpected costs.
This layered approach—combining insurance, preventive care, and financial planning—enhances resilience against escalating medical expenses.
Thus, medical inflation in India is a multifaceted challenge driven by technological advances, rising chronic diseases, growing demand for high-quality care, and increasing operational costs in hospitals. Households, particularly those in middle- and lower-income groups, bear the heaviest burden through high out-of-pocket expenditures, debt accumulation, and limited insurance coverage. The health insurance sector faces pressures to adjust premiums, manage claims efficiently, and maintain affordability, while the government must implement policies to regulate costs and expand healthcare access.
Addressing medical inflation requires a coordinated, multi-pronged approach:
1. Policy and Regulatory Interventions: Programs like PM-JAY and the National Health Claims Exchange provide financial protection, standardize pricing, and prevent inflated billing. Expansion of medical education increases the supply of trained professionals, improving the doctor-to-patient ratio and reducing consultation costs.
2. Expansion of Facilities and Infrastructure, Especially in Government Hospitals: Increasing capacity in government hospitals, adding more beds and ICUs, upgrading diagnostic and laboratory services, and improving telemedicine networks can reduce patient congestion, shorten waiting times, and ensure timely access to care. Investments in modern equipment, efficient infrastructure, and emergency care units in public hospitals enhance service quality, provide affordable treatment to larger populations, and help control long-term costs.
3. Quality and Standards of Care: Promoting accreditation programs, standardized treatment protocols, and continuous training of medical personnel ensures consistent, high-quality services, reduces treatment errors, and improves patient outcomes, which in turn mitigates additional healthcare costs from complications or prolonged illness.
4. Preventive Healthcare and Public Awareness: Emphasizing early detection, lifestyle modification, routine check-ups, and vaccinations helps reduce the incidence of severe diseases, lowering the burden on hospitals and household expenditures.
5. Individual Financial Preparedness: Comprehensive health insurance, emergency health funds, and strategic budgeting for medications, consultations, and wellness programs create a resilient financial defense against rising medical costs.
By combining system-level reforms, expansion and improvement of government hospital facilities, quality enhancement, preventive care, and personal financial planning, India can address medical inflation effectively. These measures will help ensure that healthcare remains accessible, affordable, and of high quality for all segments of society, protecting both the health and financial well-being of its citizens.
(Dr. Manoj Kumar Paul, former Principal, Women’s College Silchar, Assam)




